The Professional’s Guide to Ultrasound
You’re buying ultrasound equipment for your practice. It’s pretty bewildering. You know the basic buyers’ rules. You should narrow your choice based on whether you’ll be using general applications, or vascular work, or OB/Gyn, or cardiac. These are the usual four categories.
You also know that much depends on your office set-up. Do you just want to learn a couple of applications, or do you need a machine to do TEE and mitral inflow measurements and TDI? Are you doing endocavitary at all? Are you going to bill for images, and if so, do you need to print them easily, or interact with some EMR? Are the machines really just there to guide your management? Are you teaching? Are there machines your department is already familiar with? Do you want something compact, to get around furniture or beds? If you get a portable machine, might it be stolen?
And you also know not to buy blind. Some people like to narrow down to 2-3 options and then get the techs from these companies to come demo. So you’re planning on doing this. Some of them bring pretend-patients. Demos should be on living people, you’re aware. And you know you should have the decision-maker on hand to watch.
But you still don’t feel good.
It’s a complicated situation for a lot of buyers these days, particularly as point-of-care ultrasound takes center stage. It’s great that ultrasound is immediately on hand, but the machines in general use may not be of good enough quality to answer clinical questions. The operator may not really understand the anatomy, or recognize artefacts or anomalies; there can be counter-productive false diagnoses. Point-of-care is even its own culture in a lot of ways. It’s not like having radiologists involved. It’s more like a haphazardly-trained militia of nearly amateur users. Even storing the images may not be practical, in point-of-care, because the infrastructure is bought piecemeal. Maybe you’re buying equipment for a largely improvised setting just like this, and then having to explain it all to the people who are using it.
Sales teams probably aren’t going to help you much. They use jargon, like 4D, coded harmonics, and code excitation. They don’t see patients. They want you to spend a lot.
So here you are. You’ve been busy in your profession, so you may not know what the jargon means, or what equipment these days can do, or what, in the end, you should buy.
Maybe you could use a quick primer.
If you’ve got five minutes, let’s give you a top-level professional’s guide to what all the ultrasound talk really means, and where it comes from. Then you’ll know what you want to get for your practice.
Ultrasound from Start to Finish
The first ultrasound system was a handheld transducer that sent signals and measured reflection. This was called ‘A-mode’. ‘M-mode’, which measured reflection as a function of time, emerged as a way of seeing motion. ‘B-mode’ was next, a two-dimensional brightness system using directional position-sensing arms. Putting three transducers on a rotating wheel, a trick learned in the 1970’s, turned B-mode into proper real-time ultrasound, much as we know it now.
Beams got better, sent and received through phased arrays of transducers. The signals were steered electronically, at focused depths, with much better resolution. The trick there was to delay sound at the focal center until it was in phase with reflections from the outer areas. Digital beamforming replaced the analog delay system.
Measuring movement by Doppler shift was a 1970’s innovation, and showing it in color comes from the 1980’s. You’ve probably used this to show blood flow in fetal hearts.
Digital arrays were then developed that can see in more than one direction. Their size reduced enough to fit down the esophagus, a nice touch if you want to see real-time heart movement in obese patients, for example.
Sound distorts as it passes through areas of changing density. So there are aberrations in returning signals. Matrix arrays are helping improve this, but these aberrations are an enduring problem. There is also interference from signals scattering during reflection. The result is ‘speckle,’ and there is no way yet to remove it completely, though machines can smooth it by combining the signals received at different frequencies and combining them. But then resolution suffers.
A recent technique to reduce signal clutter is ‘tissue harmonic imaging.’ This is when a pulse is received at twice its transmission frequency. All signals generate spurious emissions at their harmonic, as you’ll remember from college physics. That’s why there are double rainbows if the light is strong. Radio transmitters are designed to suppress the electromagnetic harmonics they generate. Returning ultrasound has better resolution at higher frequencies. Bandwidth improvements to transducers made imaging these signals possible. There’s another reason THI works so well. The imagine beam doesn’t form at the skin surface, but a couple of centimeters down. That means no interference from things like ribs and fat.
3-dimensional transducers are now pretty common. They’re steerable, electronically, so the beam can be focused optimally through the field depth, making a very thin slice than the old fixed lenses could. With the right signal processing, lots of slice images can be combined, for really smooth, detailed images. This is nice for seeing small structures.
What do you do about wide views, then? There is panoramic imaging, where the transducer moves along the patient’s outside, and blends images over long distances. There’s a cross-correlation technique that matches all these images up.
In a way, digital signal processing has turned out to be more important than transducer technology. These days systems use much the same hardware, but the algorithms change to suit the imaging situation. It means that you need to pay attention to how well your machine stores data, and how well it talks to other machines. Sometimes a doctor won’t see an image on the same machine that took the image. Venders are working to standardized formats and compression techniques. Talk to your sales representative about this.
Bulk-processing of signals is what allows 3D imaging. Showing these signals over time is what’s called ‘4D.’
Signal processing is behind ‘synthetic aperture’ techniques too, in which a very broad beam is transmitted in many directions and then analyzed. It’s extraordinarily fast, though its resolution suffers. Its quality depends on the computer processing power. Another technique is ‘pixel-oriented processing.’ This will become ever more common as computer power grows.
The latest news in ultrasound, and you’ll notice this as you shop, is the proliferation of portable systems. Early ones suffered from limited feature sets or poor resolution. Processing power and ASIC integration have improved, so portable ultrasound is now finding use in places where car-based machines can’t easily go. Emergency departments and ambulances use them a lot, for example. There are even quite serviceable instruments than be carried in coat pockets.
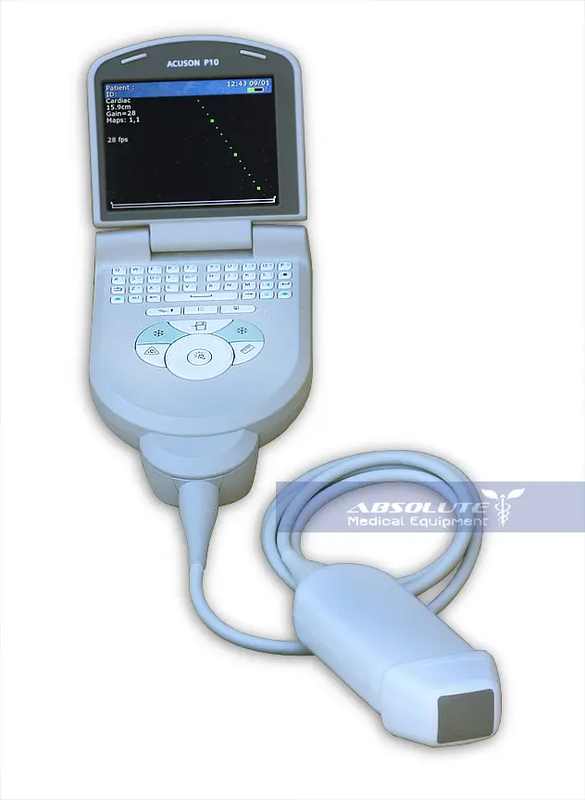
Portable systems vary quite a bit. If you’re shopping with us, you might have a look at the popular GE Logiq V2. It’s engineered for speckle reduction, and operators like its ergonomics and its intuitive, work-reducing keystroke design. Even more portable, and also popular, is the Siemens Acuson P10. This is a pioneering handheld device, in use in cardiology, emergency medicine, and obstetrics. You use it when you’re in a hurry. It’s a quick way to get past the usual departmental delays. It’s also good for routine follow-ups, when you could spend a lot of time, but you know you don’t need to.